最近,许多国家遭受了全球金融危机的影响[1]。Major economic problems have been faced by low and middle income countries; however, even some European Union nations (such as Greece, Spain and Italy) are experiencing the effects of the global crisis [2]。
几位专家指出,政府专注于卫生系统的国际政府和非政府组织的经济资源有限:急剧减少了许多急性和慢性疾病的资金,无法改善医疗保健组织,无法取代离开工作的人员(例如迁移到富裕的国家或退休),无法将新的诊断,治疗和预防方法转移到日常常规临床和公共卫生活动中。这种情况的最相关结果是一些疾病的负担增加(诊断和/或治疗和/或预防)[3–5]。The highest risk of a difficult-to-recover picture is associated with increased probability of transmission of infectious diseases.
At this point in time it is crucial to develop a strategy of health priorities based on accurately evaluated epidemiological and financial burdens of the most important diseases.
Tuberculosis (TB), one of the main global health priorities with about 9 million estimated new cases and 2 million deaths, together with HIV/AIDS and malaria, creates major economic problems in high burden countries and among affected communities [6]。已经对结核病的医疗保健负担进行了几项研究,以及系统的评论和荟萃分析,包括更严重的结核病形式,例如耐多药TB(MDR-TB)[7–12]。
The World Health Organization (WHO) and its partners are finalising the latest version of the new post-2015 TB control and elimination strategy, which will be discussed at the World Health Assembly in May 2014 [13,14]。随着将无结核病的世界留给后代(零死亡,疾病和与结核病有关的痛苦)的愿景,以及结束全球结核病流行的目标,新的WHO战略对2035年有雄心勃勃的目标(如图。1):1)TB死亡人数减少了95%(与2015年相比);2)结核病的发病率降低90%(每10万人口<10 TB病例);3)没有受影响的家庭因结核病而面临灾难性费用。
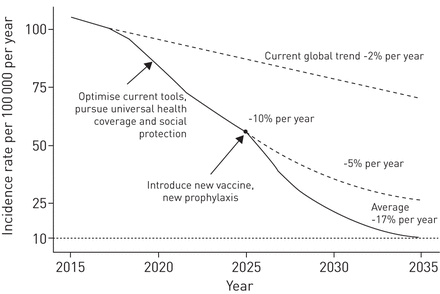
估计全球结核病发生率的减少。经发布者的许可重复[14]。
新策略建立在三个核心支柱围绕:1)以:1)综合,以患者为中心的护理和预防,2)大胆的政策和支持系统,以及3)加强研究与创新(表格1)[14]。
虽然第一个支柱将捕获点中描述的核心技术原理和停止结核病策略(快速诊断,筛查处于危险中的人群,治疗和患者支持,包括MDR-TB,TB/HIV和合并症,诊断和治疗,诊断和治疗。,疫苗接种),第二支柱将捕获支持这些原则的必要政策(政治承诺和足够的资金,社区的参与,民间社会组织和所有医疗保健提供者,以及卫生服务的整合;全面的健康保险;用于案件通知和案件通知和案例通知和监管框架改善了重要的统计数据,感染控制和质量抗结核药物的基本原理;社会保护,缓解贫困和与社会决定因素作斗争)。最后,第三个支柱将进一步刺激新诊断,药物和疫苗的研究和合理使用。
However, until now, studies investigating the impact of TB from the patients’ perspectives are rare and no systematic review on medical and non-medical costs, as well as income loss (and its drivers) for TB patients and affected households in different settings is available in the scientific literature.
In this issue of the欧洲呼吸杂志,tAnimuraet al. [15focu]系统综述研究sed on the direct (out of pocket) and indirect (opportunity) costs of TB, including income loss incurred by TB patients, and their coping strategies [15]。正如作者在引言中指出的那样,普遍的健康覆盖范围(“无需为其支付经济困难的必要卫生服务的普遍接触”)和社会保护以“疾病时收入更换和社会支持”是支持该公司的关键原则该研究的理由。
This study is a first step in providing information that can be used in trying to meet the tentative global targets for the WHO strategy that no TB-affected family will face “catastrophic costs due to TB”, globally, by 2020 [16]。
自2011年以来,全球结核病控制议程的先前文件中存在这些原则[17–21]。不幸的是,他们更专注于确保免费结核病诊断和治疗(并在本地项目中提供激励措施/推动力),而不是实施涵盖直接医疗费用超出直接医疗费用的系统(例如损失收入的赔偿viasickness insurance, disability grants, other conditional or unconditional cash transfers, food assistance, travel vouchers, and other support packages). The ongoing global crisis is, of course, not facilitating the implementation of these principles [3–5,22]。
TAnimuraet al. [15]实施了一种从时间标准中全面的搜索策略,但仅专注于低收入和中等收入国家,i.e.on the countries mainly suffering the epidemiological burden of this infectious disease. They selected 49 original studies.
在进行的25项研究中,主要的经济比例损失(最佳估计60%,范围16-94%)与丢失的收入有关,其次是医疗费用(最佳估计20%,范围为0-62%)和非医疗费用(最佳估计为20%,范围为0-84%)。这里介绍的八项研究表明,间接成本是抗TB药物治疗之前和治疗期间的重要驱动因素。由于患者的总体支出中有50%发生在治疗开始之前,因此早期诊断和立即开始抗TB方案可以立即节省资源。
Drug costs form a substantial part of the direct medical costs (34% on average), followed, in order of importance, by tests prescribed at diagnosis and during follow-up (27% on average) and by hospitalisation costs (24%).
Unexpectedly, findings from 16 studies presenting disaggregated data for direct and indirect costs highlighted the relevance of food and transportation to the nearest TB service on indirect costs (50% and 37%, respectively).
One of the most striking results of the study analysis is the average “price” the patient pays for his/her TB disease: 847 and 379 US dollars represent the unweighted total mean and median cost of TB, respectively.
总成本分别占个人和家庭收入的44%和23%(由于数据分布偏差,作者包括中位数值)。没有通过性别分层检测到差异,只有少数例外。该研究的一个重要发现是“在治疗过程中最大程度地减少成本并不能保证(如上所述)的财务风险保护,因为在治疗开始之前,通常会发生很大一部分费用。”诊断和治疗启动的时间似乎是成本达到顶峰的地步。
如作者所建议的那样,减轻此期间发生的费用,例如,通过更负担得起的医疗服务和社会保护计划,可能是一种有力的干预措施,同时将减少诊断的延迟并改善获得结核病护理的机会。
主要成本会影响最贫穷的不成比例。总而言之,最常见的应对活动是:使用储蓄,借贷以及出售个人和家居用品。
Only a few studies (i.e.three) evaluated the financial consequences of MDR-TB: MDR-TB is, in fact, economically disastrous for the total and indirect costs generated when compared with drug-susceptible TB.
作者建议,两组患者,即贫困和MDR-TB患者,都需要医疗保健和社会保护系统的特别关注。
The study results could be affected by some methodological shortcomings, as the authors correctly underlined: 1) publication and selection biases, as the analysis was performed mostly on studies dealing with diagnosed patients and managed in the public sector; 2) great heterogeneity in design and methods of the studies analysed, as well as in the presentation of their results; and 3) limited information on the context of the study, such as on details of the local health system.
However, the main strength of this study is its originality: for the first time a systematic literature review on TB patient costs was performed.
The study underlines the importance of several economic drivers, including indirect costs, particularly those before treatment starts, as well as hospitalisation of (contagious) patients. More stratification, for example on gender and types of TB, including MDR-TB, would be useful in future studies.
需要尽快就结核病患者费用进行更多研究:他们将向政客和其他利益相关者提供有关资源最佳分配,卫生和社会保护系统的关键差距以及患者和医疗保健提供者的潜在节省的相关建议。可能会受益。基于这样的研究决定政策决策将有助于在资金不足的时代合理地分配财务资源。
In conclusion, this study presents the necessary background evidence to support the new WHO post-2015 strategy which is focused on TB elimination [13,22]。To reach TB elimination we need all described interventions in place with particular attention to vulnerable populations and the capacity to tackle the social determinants of health [23,24]。
Footnotes
Conflict of interest: None declared.
- 已收到2014年4月5日。
- Accepted2014年4月7日。
- ©ERS 2014















