To the Editors:
Pulmonary tumour embolism is considered to be a rare cause of pulmonary hypertension. The incidence, studied in autopsy series, varies from 3 to 26% of patients with solid tumour [1]. It occurs most frequently in breast, stomach, lung, liver, prostate and pancreas adenocarcinoma [1]. The literature shows a male predominance and an average age of 52.4 yrs [2]. The signs are those of any pulmonary hypertension, occurring either during the history of a known neoplasia or as the first manifestation of malignancy. Pre-mortem diagnosis is difficult to confirm and definitive diagnosis is usually made on an autopsy study. Several studies have reported pulmonary wedge aspiration cytology performed during a right heart catheterisation as a useful pre-mortem diagnostic tool [3]. Treatment consists of treating the neoplasia. Specific treatment for pulmonary hypertension has not been evaluated. Most frequently, evolution leads to refractory right cardiac failure and death [4]. In rare cases improvement has been reported after chemotherapy [5] or endarterectomy [6].
两种机制可以参与肿瘤肺栓塞肺动脉高压的发育:第一个是通过多发性肿瘤微明的小肺动脉机械闭塞,第二个是通过肺肿瘤血栓形成微盲(PTTM)的发展与胎儿细胞的内皮相互作用。在PTTM中,激活炎症和凝血途径,导致血管改造现象,肺动脉源性系统的弥漫性变窄[7]. The role of tissue factor and vascular endothelial growth factor [8] as well as platelet-derived growth factor in the pathogenesis of PTTM has been highlighted by previous studies.
我们举报了一个49年代的女性患者,涉及怀疑肺动脉高压。这一集发作开始4个月前进行运动诱导的呼吸困难的投诉。肺血管造影计算机断层扫描(CT)发现没有肺栓塞。超声心动图显示出收缩肺动脉压的轻微升高,导致对高血压性心脏病的可能舒张功能障碍的诊断。患者对全身高血压的医疗得到加强,没有进行进一步的探索。
Due to disabling dyspnoea, the patient was hospitalised 4 months later. No signs of cardiac dysfunction were seen, the pulmonary auscultation was clear. Pulmonary embolism was eliminated by a pulmonary angiographic CT but rare ground-glass opacities were noticed. The echocardiography revealed signs of chronic cor pulmonale with dilatation of the right cavities and severe elevation of the systolic pulmonary artery pressure at 70 mmHg. The bronchoalveolar lavage showed intra-alveolar haemorrhage and no malignant cells, the pulmonary function tests were normal, the viral serologies and complete immune check-up were negative and the abdominal echography showed no sign of portal hypertension. Given the association of rapidly evolving pulmonary hypertension, alveolar haemorrhage and ground-glass opacities a possible pulmonary veno-occlusive disease was suspected [9]. The patient was addressed to our unit (Pneumology, Hospital CHU de Nantes, Nantes, France) for further investigations.
The right cardiac catheterisation revealed severe pulmonary hypertension with an elevation of mean artery pulmonary pressure at 62 mmHg, diminution of the cardiac output (3.36 L·min−1) and of the cardiac index (2 L·min−1·m−2),并在16.7个木装置上增加肺血管抗性。肺楔压未升高(6mmHg)。在程序期间没有进行细胞学研究。由于低血压和意识丧失,患者被转移到重症监护病房。开始用多番番葡萄酒,去甲肾上腺素,Epoprostenol和一氧化氮进行处理,无需改善。解释为严重肺动脉高压症的血小板减少症出现在血液测试上。鉴于患有严重低心的迹象的戏剧性演变,患者在oro-气管插管后的静脉动脉体外膜氧合下,并在紧急移植清单上刻。她在入院后6天受益于心肺移植。
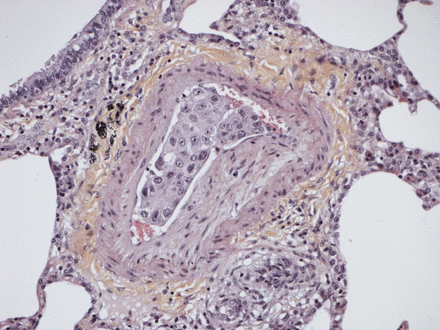
Rapidly a graft dysfunction associated with a multiorgan failure was observed. The anatomo-pathological examination of the explanted lungs showed tumoural cells within the pulmonary arteries associated with extensive intimal fibrosis consistent with PTTM (fig. 1). Following physical examination, an abnormality of the left breast and an axillary left lymphadenopathy were found. Blood tests showed a high level of the tumour marker CA 19-9. The CT scan confirmed a growth in the left breast associated with bilateral axillaries adenopathies and a left supraclavicular adenopathy. Biopsies of these lesions were performed revealing breast adenocarcinoma. A medullar invasion explaining the initial thrombocytopenia was revealed by a bone marrow examination.
Fibromuscular intimal thickening leading to reduction of the lumen of the pulmonary arteriole. There is an accumulation of carcinomatous cells in the residual lumen. Haematoxylin and eosin stained, original magnification ×40.
预后不良导致限制特异性护理。患者在移植后17天死亡。
This case is important because breast cancer was not diagnosed due to the rapid evolution of the pulmonary hypertension and the need for emergency transplantation. Pulmonary hypertension was the first and only sign of malignancy. Neoplasia was not evoked due to the young age of the patient, absence of self-reported clinical signs and no specific findings on the CT scan. Retrospectively, it was found that a mammography conducted a few months earlier showed a lesion on the left breast (ACR 2). A new evaluation of the pre-transplant CT scan revealed a lesion of the left breast and a left axillary adenopathy (fig. 2).
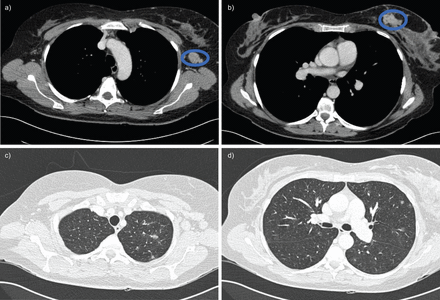
预移植预移植增强的计算机断层摄影图像显示左乳房的病变,左腋窝腺肿和稀有磨玻璃结节。a)纵隔窗口切割显示左腋窝腺病变。b)纵隔窗口切割显示左乳房的病变。C和D)薄壁窗切割显示稀有磨平玻璃结节。
The case also highlights the importance, for all patients, of a complete check-up before transplantation, including the search for a neoplasia. Indeed, when dealing with severe pulmonary hypertension, the possibility of a malignancy should always be kept in mind as it can lead to transplantation being reconsidered. In this case, the check-up failed to show any signs of malignancy even though the CT scan was pathological, emphasising the importance of a rigorous and complete analysis of the various imaging. The patient should have benefited from a gynaecological consultation as normally conducted before any transplantation but the rapid respiratory failure resulted in an incomplete pre-transplant evaluation. Moreover, development of a subacute pulmonary hypertension with rapid evolution towards right cardiac failure may be an indicator of malignancy.
Consequently, neoplasia should be considered when faced with any unexplained, rapidly developing, pulmonary hypertension.
脚注
兴趣表
A statement of interest for D. Horeau- Langlard can be found atwww.www.qdcxjkg.com/site/misc/statements.xhtml.
- ©ERS 2012